If you are experiencing growth of hard lump or protrusion near premolar or canine, it could be torus mandibularis— also called tori. It is not uncommon, as the prevalence rate is 12.3% to 26.9%, particularly among people in their forties. The prevalence of sublingual protuberance is relatively high among males. Though the cause of tori growth is not clear, scientists link it to masticatory hyperfunction, genetics, and diet. In most cases, nodular bony growth remains less than 2 mm in size of varying shape. Although it is not cancerous or harmful, you should consult your doctor to know about the reason, as it could be due to other medical conditions.
What is Torus Mandibularis?
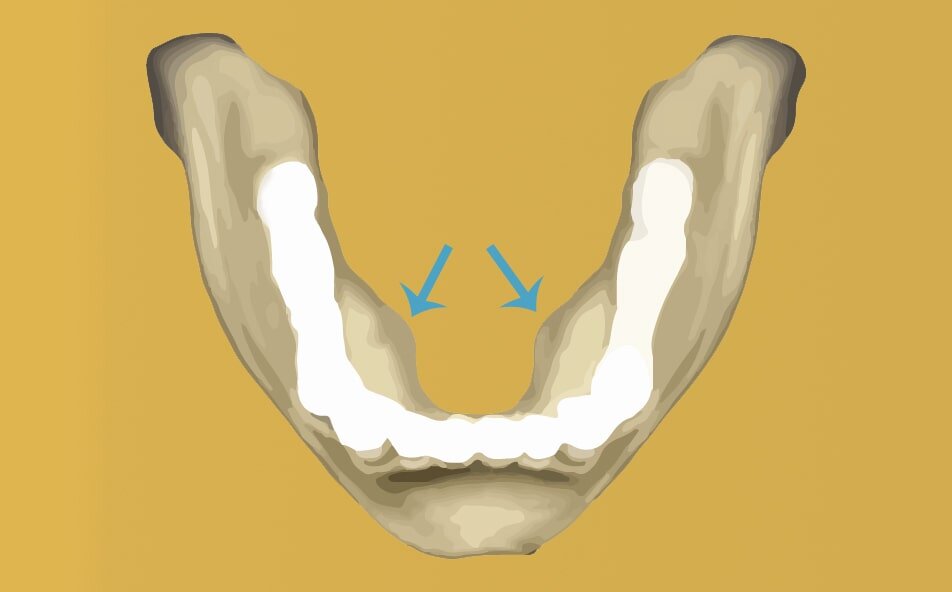
A bony growth in the mandible (tongue side of the jaw), mostly near premolars, and above mylohyoid muscle mandible attachment is called Torus mandibularis. The shape varies from person to person, but it could be either bilateral or unilateral, and multiple or singular. However, in 90% of cases, tori grows bilaterally. Similar bone growth near the midline of the palate is called torus palatinus. Tori can also grow on the cheek (buccal side) of the lower and upper teeth. Torus is not harmful and doesn’t require removal, but if it interferes with a dental prosthesis, your doctor might recommend removal for better fitting.
Symptoms of Torus Mandibularis
Torus mandibularis, or rather any other tori, grows gradually, and people fail to notice minor symptoms as it remains painless. The dental system is highly sophisticated, so the growth of a hard lump will naturally affect oral functions. You might experience these symptoms with a bony protrusion extending from the premolar area:
- Growth of single or multiple hard lumps on the tongue side of the jaw near premolars
- The gradual growth of the painless bump
- It affects the fitting of orthodontic devices or mouth guards
- If tori grows larger, it might cause speech impairment
- The presence of tori make it difficult to fit dentures and aligners
- You might experience difficulty in chewing, especially when tori is near teeth
- Protrusions will naturally catch food particles, thus making your mouth susceptible to bacterial infections.
If you are experiencing symptoms like fever, swelling, ulcers on the gums, pain, along with illness, then it could be something other than a torus mandibularis. You won’t feel pain and discomfort with tori, but you should get in touch with your dentist and discuss all possible issues to keep the dental system healthy.
Causes of Torus Mandibularis
Tori mandibularis is very common in the US, as the incidence rate is over 25%, particularly among people of Inuit and Asia descent. Studies conducted on twin subjects suggest that torus is mostly genetic. However, experts believe it could be due to factors including:
Age: Torus mandibularis, or rather any tori, is more common among people over 40 years. Although tori start developing at an early age, bone growth becomes visible once people hit their forties.
Dental Structure: Incidence of tori is high among people with complicated dental structures with teeth misalignment and bite issues. The risk of tori occurrence increases manifold with crowded teeth.
Genetics: Finding of some recent studies conducted on twins suggest that bony outgrowth in the mouth has a strong genetic link. Although exact factors causing tori are not known, the genetic link is exceptionally high, 93.6%, among identical twins.
Grinding: If you have the habit of teeth grinding, the chances of bony growth in the mouth are relatively high. Aggressive grinding and clenching create pressure imbalance of dental structure. Experts believe aggressive grinding could trigger bony outgrowth. However, there is no consensus.
Bone Density: If your bone mineral density is high the chances of the development of a hard lump or protrusion in the mouth is higher. Research shows that among postmenopausal white women with tori the bone density was relatively high.
Diet: Another study links bone growth to high consumption of polyunsaturated fats and Vitamin D. If you are consuming a large amount of saltwater fish, the risk of torus mandibularis is relatively high.
What Are the Treatments for Torus Mandibularis?
Torus mandibularis, whether single or multiple, is usually harmless, and treatment is not recommended if it is not affecting your day-to-day life. If tori is affecting your speech, swallowing ability, oral hygiene, or fitting of orthodontic devices, your dentist might recommend removal. In some cases, like denture fabrication, it might be necessary to remove tori surgically for better fitting of the device.
If the bony protrusion is at such an angle that it makes chewing painful, surgery might be a good option as it will help you get rid of a lifelong challenge. This surgery is performed by someone who specializes in treating the face, neck, and jaws. You will be administered local anesthesia, and then your maxillofacial surgeon will make an incision on the tongue side of the jaw and remove the hard lump. Once done, the surgeon will close the opening with dissolvable sutures.
It takes around 30 minutes to perform the tori removal surgery, and the risk of complications is low. However, complications might occur, which could be:
- Minor injury to the palate and nasal cavity
- Infection in the affected area
- Swelling
- Blood loss
Just like tooth removal surgery, healing after tori removal surgery also takes 3 to 4 weeks. Your surgeon will suggest measures to prevent infection so that recovery could be faster and painless. Follow instructions and continue taking medication, as prescribed, and maintain standard oral hygiene to heal quickly.
When to see a doctor?
Just like any foreign object in the mouth, you will feel the growth of bony protrusion if the torus mandibularis is big enough. If you regularly visit the dentist, he will notice bony outgrowth before you start experiencing the symptom. Swelling could be due to other medical conditions, so don’t ignore if you notice any unusual growth in the oral cavity. Although torus mandibularis isn’t harmful, it is better to seek advice from professionals and remain free of the anxiety created by uncertainty. Consult your dentist if:
- You notice the development of a hard lump in the mouth
- The bony outgrowth becomes painful
- You are experiencing difficulty in swallowing or speaking
- Growth is changing size and color
- It is affecting your orthodontic appliances
Is Torus Mandibularis Cancer?
No, it is not cancer. However, you should get it examined to remain free of the worries of cancerous growth. Oral cancer is rare, and even if it occurs, it usually develops on the soft tissues of the cheeks and tongue. Your doctor will recommend a CT scan to rule out possibilities of cancer.
Does Torus Mandibularis Go Away?
Bony outgrowth in the mouth doesn’t go away naturally. So, if your hard lump growth isn’t showing symptoms, you should consult your dentist. In most cases, he won’t recommend removal. But, if it is affecting your speech and swallowing, he could suggest surgical removal of bony outgrowth by a specialist surgeon.
Is Torus Mandibularis Bad?
Torus mandibularis of normal shape and size is harmful. But, if it is large, it might interfere with your speech and eating abilities. A similar type of outgrowth could be due to other medical conditions, so you should better seek professional intervention to get rid of anxiety caused by unusual growth.
Can a Dentist Remove Tori?
Although tori are harmless, if the bony protrusion is interfering with daily life, your dentist might recommend removing the hard lump. Performing oral surgeries need a special type of training, so you should consult a maxillofacial surgeon—a specialist trained for facial, neck, and oral surgeries- for tori removal. Although it is less complex than removing wisdom teeth, it is better to get tori removed by a maxillofacial surgeon.
Can Tori Cause Jaw Pain?
If the bony protrusion is at a troubling angle, it might get injured by hard food items. The injury could get infected by harmful bacteria, thus causing inflammation and pain in jaw areas. In some cases, it could cause gum inflammation and mild pain. Usually, infections subside with normal saltwater rinse, but if it sustains for long you should seek dentist advice to control pain and inflammation.
Does Torus Mandibularis keep growing?
In most cases of tori, the nodular bony growth remains less than 2 mm in size of varying shapes. But in some cases, it could grow bigger and start impairing speech and eating abilities. If your tori is growing, you should get in touch with your dentist and get them removed to bring your oral space in shape.
How much does tori removal surgery cost?
The torus mandibularis treatment, including removal surgery, cost varies depending on the expertise of your doctor, location, and of course your insurance coverage. The cost of removing single torus mandibularis in the US averages around $600. The cost of tori removal surgery is covered under Medicare, so you have to pay only 20% of the cost of surgery if medically necessary.
How long does it take to recover from tori surgery?
Tori is harmless, but removal will ease your discomfort. Just like any oral surgery, it takes an average of 3-4 weeks to heal effectively. You will have a functional mouth in just a few days, but you have to follow preventive measures as suggested by the surgeon to heal faster.
Outlook
Experiencing something unusual growing in the mouth can make anyone anxious. Although torus mandibularis is harmful, you should get it examined as bony outgrowth could be due to other medical conditions as well. If you have a family history of tori growth or have a complex dental structure, you should take extra caution and avoid doing things that could cause bony protrusion in the mouth. If your dentist recommends tori removal, you should better consult a maxillofacial surgeon for tori removal surgery.
Source:
- Johnson, C. C., Gorlin, R. J., & Anderson, V. E. (1965). Torus mandibularis: a genetic study.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1932651/ - Morita, K., Tsuka, H., Shintani, T., Yoshida, M., Kurihara, H., & Tsuga, K. (2017). Prevalence of torus mandibularis in young healthy dentate adults.
https://www.sciencedirect.com/science/article/pii/S0278239117305001 - Woods, G. M. (1995). Mandibular tori as a cause of inability to visualize the larynx.
https://journals.lww.com/anesthesia-analgesia/fulltext/1995/10000/mandibular_tori_as_a_cause_of_inability_to.37.aspx